For my journal article on gingival diseases, I chose "Self-reported gingival conditions and self-care in the oral health of women during pregnancy" by the Journal of Clinical Periodontology. The objective of this study was to describe the self-assessment of gingival health conditions in pregnant women, their oral hygiene behavior and dental visiting habits, and to analyze self-care practices of pregnant women in relation to perceived gingival problems.
Gingival Disease: Pregnancy-Associated Gingivitis
What is Pregnancy-Associated Gingivitis?
Pregnancy-associated gingivitis is an exaggerated inflammatory response of the gingiva to dental plaque biofilm and hormone changes usually occurring during the second and third trimesters of pregnancy. Significant differences are found between the
gingival conditions of women during pregnancy and after delivery. It is important for pregnant women to be aware of this gingival disease and take extra care of their oral health to prevent this from happening. Also, there have been recent major studies stating that there is a link between pregnancy-associated gingivitis and premature birth.
Distinguishing diagnostic factors
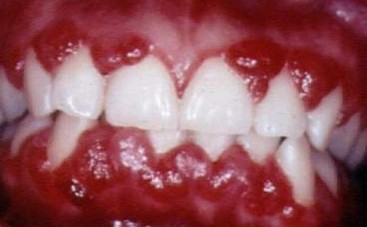
A pregnant woman experiencing gingivitis may have edematous and dark red gingival tissue, with bulbous interdental papillae (as shown in the image above). Usually this gingival inflammation appears between the second and eighth month of pregnancy, and can range from mild to severe diagnostic factors of this gingival disease. For example, the gingival tissue could be reddish with light bleeding when brushing, or there may be severe swelling and bleeding of gum tissue. In some cases, a gingival papilla can react so strongly to bacterial plaque biofilm that a large, localized overgrowth of gingival tissue may form on the interdental gingiva or gingival margin. This is known as a pregnancy-associated pyogenic granuloma or pregnancy tumor. Don't let the word tumor scare or fool you! This mushroom-shaped gingival mass is noncancerous and usually painless. Although, the tissue mass may bleed easily if disturbed and can appear to be covered with dark red pinpoint markings. Pregnancy tumors usually disappear on their own after the baby's birth.
Etiology of the disease
Etiological factors of pregnancy-associated gingivitis are primarily related to hormonal changes and bacterial dental plaque. As described in my journal article, the etiology of gingivitis during pregnancy is shown to be complex. Firstly, changes in the bacterial flora of the dental plaque biofilm are found even with no increase in the amount of dental plaque. Poor oral hygiene can also be a factor due to the build-up of plaque causing this exaggerated inflammation. Secondly, as stated in this article from the Journal of Clinical Periodontology , "during pregnancy higher levels of progesterone and estrogen in blood appear to affect the permeability of the blood capillaries in the gingiva, and thereby increase the susceptibility to gingival inflammation due to bacterial, physical, and chemical irritation."
Pathogens associated with the disease
From 1,000 to 100,000 bacterial species can be cultured from an individual site with gingivitis. There are no specific pathogens for this gingival disease but most cases of gingivitis consist of almost equal portions of Gram-positive and Gram-negative bacteria. Tissue associated plaque biofilm contain Gram-negative cocci and rods. There is a predominance of species such as S. oralis, Streptococcus intermedius, P. gingivalis, P. intermedia, T. forsythia, and F. nucleatum.
Classification of the disease
According to the AAP Classification of Periodontal Diseases and Conditions, pregnancy-associated gingivitis would be 1A, classified as dental plaque-induced gingival diseases.
Prevalence of the disease
Between 50%-70% of women will develop gingivitis during pregnancy.
Patient education
- Brush at least twice a day, especially after vomiting from morning sickness
- Floss at least once a day
- Keep scheduled professional cleanings, and discuss any problems with the dentist
- See the dentist at least once during pregnancy
Treatment recommendations
- Use a daily warm salt rinse
- Use a soft toothbrush to cause less irritation to the gums
- If the pregnancy tumor doesn't disappear after child birth, surgical removal is recommended.
Maintenance recommendations
According to my article, most authors conclude that gingival problems during pregnancy can be reduced considerably if the subgingival plaque is kept at a low level, and suggest that dentists play an important role offering oral health education and plaque control to their pregnant patients. I would recommend my pregnant patient the following:
- Good oral hygiene, plaque and calculus control
- Maintain frequent visits to the dentist
- Keep up on scheduled professional cleanings
References:
Christensen, L., Jeppe-Jensen, D., & Petersen, P. (2003). Self-reported gingival conditions and self-care in the oral health of Danish women during pregnancy. Journal Of Clinical Periodontology, 30(11), 949-953.
Nield-Gehrig, J. S., & Willmann, D. E. (2011). Foundations of periodontics for the dental hygienist. (3rd ed.). Philadelphia, PA: Lippincott Williams & Wilkins.
**All images received from google image
Christensen, L., Jeppe-Jensen, D., & Petersen, P. (2003). Self-reported gingival conditions and self-care in the oral health of Danish women during pregnancy. Journal Of Clinical Periodontology, 30(11), 949-953.
Nield-Gehrig, J. S., & Willmann, D. E. (2011). Foundations of periodontics for the dental hygienist. (3rd ed.). Philadelphia, PA: Lippincott Williams & Wilkins.
**All images received from google image